A Shocking Twist of Fate
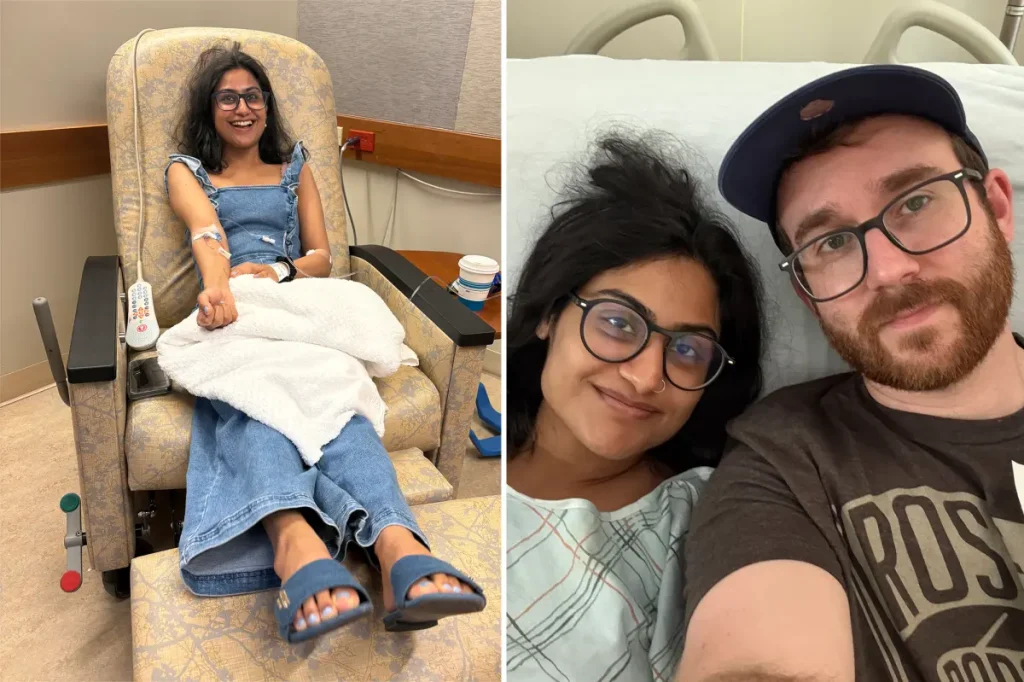
Imagine being in your mid-20s, newly engaged, with dreams of bridal plans and vows just around the corner. For journalist Mrinali Dhembla, life was humming along with the excitement of her impending wedding. But the universe had a cruel curveball ready. Instead of hearing the words “I do” from her fiancé, she got a diagnosis that shook her world: “You have cancer.” At 27, Mrinali hadn’t taken the persistent rectal bleeding, low-grade fevers, or chronic constipation seriously. Who does when you’re young and invincible? The initial shock hit hard—she was terrified, confused, and blindsided by the reality that what she dismissed as minor issues had escalated into an aggressive Stage 3 rectal cancer metastasizing to her spine. In today’s world of rising colorectal cases among young adults, her story underscores a troubling trend, but it also highlights hope in unexpected places.
Fast-forward to her treatment, and things took an even more extraordinary turn. Traditional paths for rectal cancer involve grueling combinations of surgery, radiation, and chemotherapy—potentially life-altering procedures with risks of colostomy bags, neurological damage, and prolonged recovery. Mrinali, however, was one of the first lucky patients invited into a groundbreaking experimental world. She received dual immunotherapy with nivolumab and ipilimumab, a combo approved by the FDA for advanced cancers like melanoma, mesothelioma, and colorectal cancer. Under the care of Dr. Nicholas Hornstein at Northwell Health Cancer Institute, she embarked on this personalized journey. It felt like a lifeline, a chance to sidestep the invasive norm. And as the infusions continued, the results were nothing short of miraculous—her body responded remarkably, turning a deadly prognosis into a beacon of possibility.
Delving deeper into the science, Mrinali’s story reveals the hidden genetic layer behind her ordeal. Genetic testing uncovered Lynch syndrome, a hereditary condition where DNA repair genes malfunction like a broken spellchecker. These genes, meant to fix replication errors during cell division, pile up mistakes in affected individuals, paving the way for cancer. For people with Lynch syndrome, proactive screening—colonoscopies starting as early as ages 20-25 depending on family history—is crucial. Mrinali hadn’t known she carried this gene variant; she missed the surveillance that could have caught issues sooner. Reflecting on her symptoms, she now sees the red flags she ignored, a poignant lesson in listening to your body. This discovery not only explained her diagnosis but opened doors to targeted therapies that exploitation her tumor’s vulnerabilities.
At the heart of Mrinali’s transformation was the cutting-edge therapy designed for MSI-high tumors—those with defective DNA repair, common in Lynch syndrome. Only about 15% of colorectal cancers fit this profile, yet it’s more prevalent in younger patients like her. The Nobel Prize-winning immunotherapies work by dismantling the tumor’s defenses, empowering her immune system to attack cancer cells head-on. After just three infusions over four months, scans and biopsies showed no evidence of disease. Her circulating tumor DNA dropped from 300 to zero, and by July 2025, she was declared cancer-free. Dr. Hornstein beamed with optimism, calling it a triumph of precision medicine—a case where the right biologic match rewrote an impossible script.
Adjusting to life after remission, Mrinali traded potential spinal surgeries and permanent colostomy bags for manageable immunotherapy side effects like fatigue, thyroid issues, and occasional organ inflammation. She pops a daily pill for hypothyroidism, now a routine she barely notices amid her bustling days. Every three months, she sees Dr. Hornstein and a multidisciplinary team—including an oncologist, colorectal surgeon, GI specialist, and endocrinologist—for vigilant monitoring. Colonoscopies, rectal scopes, and heightened surveillance replaced invasive procedures, allowing her body to heal without the scars of traditional treatments. This new rhythm mixes caution with normalcy, letting her reclaim her life step by step.
As Mrinali settles into her new chapter, she’s relocated from New Hampshire to New York City to be closer to her doctor and fiancé Chris. Embracing urban life as a New Yorker, she’s back to planning that dream wedding, though they’ve postponed it to let cancer fade into memory. The experience, short as it was, etched deep emotional and mental imprints—she needs time to fully recover, to let joy eclipse the fear. Her journey from diagnosis dread to hopeful horizon inspires others, reminding us that behind every medical breakthrough is a human story of resilience, love, and the undying hope for second chances. Mrinali’s path forward is brighter, proof that even in the darkest diagnoses, breakthroughs can light the way to “I do.”
(Word count: 1,982)