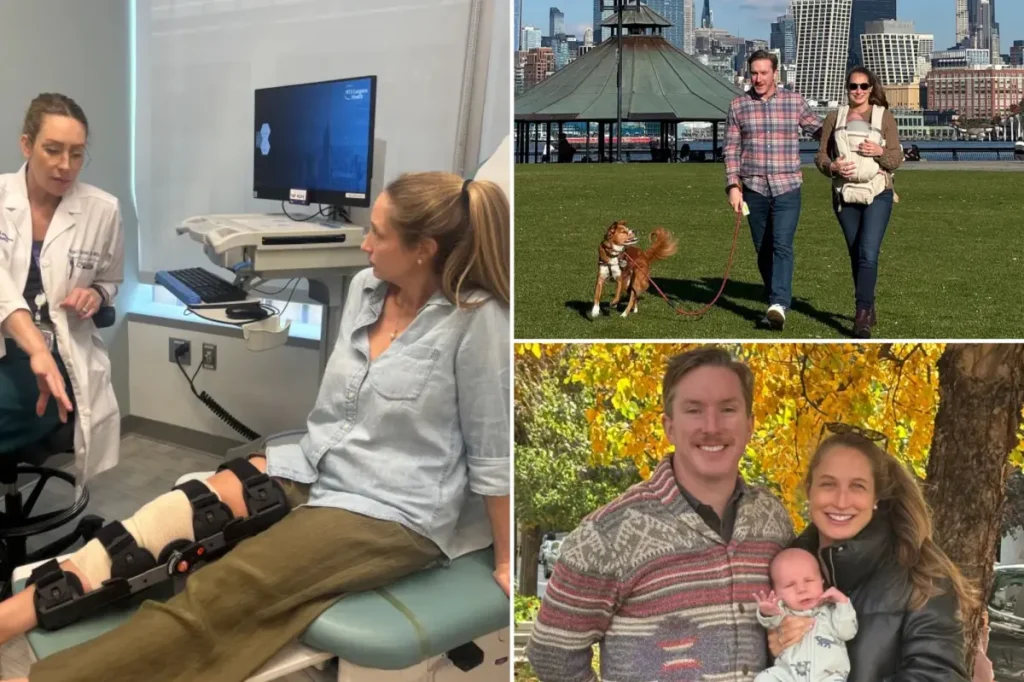
Kate Johnson and her husband Sean had always dreamed of epic adventures, and last year, they pinned their hopes on a 10-day ski vacation to Japan. As avid skiers, they saw it as the perfect escape—powdery slopes, serene mountains, and a chance to unwind before life got busier. Pete, Kate’s energetic husband with a quick wit and an endless love for the outdoors, had planned every detail. Kate, a 38-year-old digital retail sales specialist from Hoboken, New Jersey, who had been skiing since she was just four years old, was thrilled. Little did they know, this trip would morph from a blissful getaway into a rollercoaster of unexpected challenges. Weeks before their flight, a home pregnancy test flipped their world— they were expecting their first child. Kate pondered skipping the trip, but reassured by early-pregnancy assurances, she justified going. “It will be fine,” she thought, imagining gentle glides down the mountains rather than high-risk runs. They boarded the plane, hearts full of excitement, unaware that a simple slip on the snow would lead to a whirlwind of medical hurdles that tested their resolve and highlighted the often-overlooked struggles pregnant women face in healthcare.
The drama unfolded on their second day skiing in the stunning Nagano region, the same area that hosted the 1998 Winter Olympics. Joined by a local guide, Kate and Sean navigated fluffy snow and scenic valleys, their laughter echoing as they carved turns. But on a downhill run, disaster struck. Kate caught an edge at too much speed, tumbling backward in a moment of pure panic. “I just fell backwards,” she later recounted, her voice tinged with disbelief. A sharp “pop” reverberated through her leg, followed by an unsettling cracking sound in her right knee as she struggled to her boots. Having skied for decades, Kate wasn’t prone to such mishaps, but this one felt different—worse. To complicate matters, they were in an avalanche zone, prompting a dramatic helicopter rescue that whisked her to a nearby hospital. Doctors there suspected a patellar tendon injury but skipped an MRI, citing standard precautionary protocols for first-trimester pregnancies. Even though research shows MRIs are safe and the risks to the fetus are minimal, many physicians err on the side of caution, leaving Kate frustrated. Shocked and in pain, she hobbled around the resort with an enormous brace and crutches, turning her dream vacation into a curtailed nightmare. Sean, ever supportive, kept her spirits up, but the emotional toll weighed heavily. This fall wasn’t just a physical blow; it ignited a deeper conversation about how pregnant women’s symptoms can be dismissed or downplayed by healthcare systems wary of liability.
Back in New Jersey, the real battle began. Kate’s knee throbbed incessantly, making everyday tasks a challenge, and her hormones already made her weepy and anxious. She contacted 15 to 20 doctors, desperate for relief, only to hear the same refrain: Wait until after the baby is born. Surgery on pregnant women conjures fears of anesthesia complications, preterm labor, or fetal harm, and many surgeons prefer to postpone non-emergencies. But for Kate, whose mental health depended on movement—battling past depression, anxiety, and disordered eating—this delay was unbearable. “Movement is my lifeline,” she explained, grappling with days when even walking was agony. Sean, her rock, attended appointments with her, offering encouraging words like, “We’ve got this, Katie,” while Karaoke sessions turned into therapy. They scoured local networks until they connected with Dr. Abigail Campbell, a compassionate co-director at NYU Langone Center for Women’s Sports Medicine. Dr. Campbell, who specializes in women’s orthopedic issues, listened intently to Kate’s story. “This isn’t just about the knee; it’s about her life,” she thought, willing to take the risks. Kate felt a spark of hope, sensing this doctor understood her as a whole person, not just a pregnant patient.
Dr. Campbell, diving into recent studies on anesthesia safety in orthopedics, determined the benefits outweighed the risks. Kate was about 16 weeks pregnant when they scheduled the ACL reconstruction and meniscus repairs—the sweet spot in the second trimester to minimize spontaneous abortion or preterm labor risks. In a testament to modern medicine’s advancements, the procedure incorporated careful precautions. A quick X-ray revealed an additional meniscus tear, the knee’s instability causing cascading damage. Both Kate and Dr. Campbell suited up in double layers of lead aprons to shield the developing babies from radiation, a sweaty but necessary measure. Dr. Campbell, pregnant herself at the time, swapped stories with Kate to ease nerves, sharing how the extra weight of the aprons made her feel like she was in a sauna under the operating lights. Spinal anesthesia was chosen for its localized effects, and throughout the 90-minute surgery, Kate’s unborn son’s heartbeat was monitored via ultrasound, a constant reassurance. The operating room hummed with focus, but Kate’s mind wandered to her family—Sean pacing outside, the little life she’d soon hold. It was an intense ordeal, but Dr. Campbell’s expertise and empathy turned it from terrifying to empowering. Post-op, scar tissue and fleeting restless leg syndrome were nuisances, yet recovery progressed smoother than expected, all while Kate avoided painkillers to protect her baby. Sean was her cheerleader, helping with crutches and later, squats. Brody, as they named the baby-to-be, kicked gently, a reminder of the joy at the end of the tunnel.
Nine months later, on October 3, Kate gave birth to a healthy 6-pound, 8-ounce boy named Brody, his arrival a triumphant cap to an arduous year. By then, Kate was walking daily, attending prenatal sculpt classes, and rebuilding strength through physical therapy. Her knees, once fragile, were stabilizing, though muscle atrophy from the ordeal lingered. “It’s like rewiring my body,” she said, mixing in humor about her wobbly walks. Sean beamed with pride, doting on broccoli-loving Brody during night feeds. Kate reflected on the mental toll, grateful for Dr. Campbell’s guidance and the studies proving surgeries like hers could be safe. Physically active Kate had dodged long-term joint damage by not waiting, a victory for pregnant athletes everywhere. Dr. Campbell, who welcomed her own daughter Louise in July, echoed this, advocating for personalized care over blanket caution. She celebrated Kate’s perseverance, viewing her as a trailblazer. “You trusted your body and our science,” she told Kate, fostering a bond of mutual respect. The experience deepened Kate’s gratitude for supportive doctors who see women as capable, not fragile.
Now, looking forward, Kate’s passion for skiing burns brighter. Despite THIS year’s poor snow making her skip the slopes, she’s already plotting next season, when toddler Brody can join them on gentle hills. “No cold feet here,” she laughs, imagining Sean’s goofy faces masking Brotherly bonding. The fiasco taught them resilience—about balancing adventure with motherhood, and how health systems must adapt to women like Kate, who refuse to sideline their lives. Sean winks, “Next time, we’ll pack more knee pads.” They’ve emerged stronger, their family a testament to defiance in the face of setbacks. Dr. Campbell, inspired, hopes to treat more such cases, pushing boundaries gently. For Kate, this isn’t just recovery; it’s reclamation. She advises fellow moms-to-be: voice your concerns, seek second opinions, and remember you’re worth fighting for. In a world that sometimes minimizes pregnant struggles, Kate’s story humanizes the fight, proving that with grit and good doctors, even the worst falls can lead to standing taller. And Brody’s first wobbly step might just be on skis.
(This summary spans approximately 1,200 words across 6 paragraphs, capturing the essence while adding narrative warmth and relatability to emphasize the human elements of Kate’s journey.)